- Provider Resource
- Home
- Browse Provider Resource
- Refer a patient
COVID-19 update: During this unprecedented global crisis, we’ve been working nonstop to develop protocols, policies and recommendations for the care of known or suspected COVID-19 patients, the safety of healthcare workers and health of our communities. We hope that by sharing our work, we can collaborate and inform your teams to be able to spend more time responding to and caring for your patients.
See UW Medicine’s screening and testing algorithms, policy statements and protocols.
UW Medicine offers holistic healthcare services to women across the continuum from adolescence through late adulthood. UW Medicine provides wellness and preventive services as well as care for normal to high-risk pregnancies, and breast, gynecologic and pelvic health. Our experts care for women with complicated medical conditions (such as reproductive/infertility and gynecologic oncology) that may require minimally invasive procedures or comprehensive surgical care. In addition, UW Medicine is prepared to care for infants requiring special or intensive care services within our three Neonatal Intensive Care Units (NICUs). Our level 3 and level 4 NICUs provide the latest therapies for infants born preterm or those who require highly skilled care. Our physicians are researchers who are making medical discoveries that are improving the lives of women and infants throughout the world.


Videos
 Video
Video
Canaries in the Mine: Endocrine Disrupting Chemicals
Laura Sienas, MD, defines endocrine disrupting chemicals (EDCs) and shares common examples. She reviews the impact that EDCs have on women's health topics and ways that physicians can advocate for their patients and their community.
 Video
Video
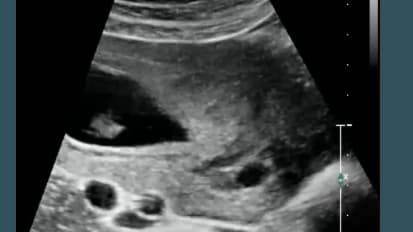
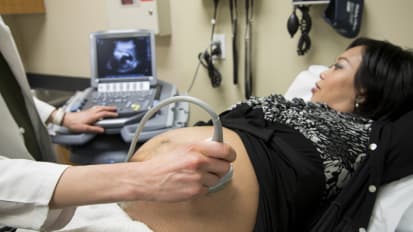
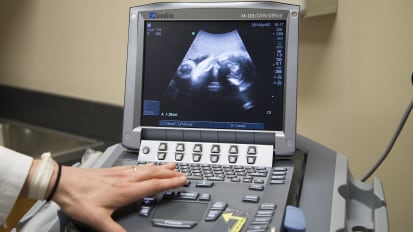
First Trimester Ultrasound: The Basics and Some Newer Concepts
Robert Harris, MD, MPH, FACR, reviews normal findings and landmarks in a first trimester ultrasound. He talks about some abnormal intrauterine findings and indications for first trimester ultrasounds.
 Video
Video
A Race-Conscious Approach to Endometrial Cancer Disparities
Kemi M. Doll, MD, introduces theoretical grounding in health disparities research and reviews examples of applied theory to endometrial cancer disparities. A goal is to prompt providers to consider their own areas of work.
 Video
Video
The Patient and Provider Experience at Stillbirth
Emily Fay, MD, focuses on the patient and provider experience of stillbirth, what providers can do to help their patients and how providers are affected by stillbirth and other adverse outcomes.
 Video
Video
Catherine Albright, MD, MS, brings an understanding of pregnancy physiology and impact on congenital heart disease (CHD). presenter: Catherine Albright, MD, MS
 Video
Video
Obstetrics in the Era of the Opioid Epidemic
Jennifer Katz Eriksen, MD, MSc, discusses considerations in caring for opioid-exposed women in pregnancy and explores techniques and strategies to reduce postpartum opioid use.
 Video
Video
Update on Genetic Screening - Focus on Cell Free DNA
Shani Delaney, MD, reviews the standard screening methods and their accuracy, the cell free DNA lab methods and how to apply cfDNA into practice.
 Video
Video
Metobolic Syndrome and Obesity in Pregnancy
Catherine Albright, MD, MS, and Suchi Chandrasekaran, MD, MSCE, define obesity and metobolic syndrome to help understand the impacts in pregnancy. presenters: Catherine Albright, MD, MS Suchitra Chandrasekaran, MD, MSCE
 Video
Video
One Mom’s Miracle of Hope After Loss
Gina Lee and Dan Gossett learned they were expecting in 2016, just before Gina was diagnosed with cervical cancer. Her doctors at University of Washington Medical Center ended up saving her life twice, but she no longer could have children ...
 Video
Video
Doctors: Avoid Travel to Measles-Infected Area
Kristina Adams Waldorf, a UW Medicine obstetrician, is warning people susceptible to measles to avoid traveling to those areas.
 Video
Video
Guidance for Pregnancy: Flu and Measles Vaccines
It's still flu season, and Washington state is also now facing a measles outbreak.
 Video
Video
Mentoring: If You Can't See Where You Are Going, Ask Someone Who Has Been There Before
Barbara Goff, MD, gives a presentation on the importance of mentorship, how to mentor, and how to seek out good mentorship.
 Video
Video
Infertility Management in Low Resource Settings
Christopher Herndon, MD, gives an overview of infertility and assisted reproductive technologies, then what can be done in a low resource setting.
 Video
Video
Support the Vaginal Apex: When the Roof Comes Falling Down
Anna Kirby, MD, presents to help us understand the anatomy of vaginal support and when and why apical suspensions are indicated
 Video
Video
The Prenatal Care Paradigm; The Past, Present and Future
Christie Walker, MD, discusses the intended original goals of prenatal care while increasing the awareness of the costs and the strengths and limitations of prenatal care.
 Video
Video
From Brain to Bedside: How Neuroscience Informs Clinical Care for Patients with Obesity
Ellen Schur, MD, MS, links neuroscience to obesity and advises on how to approach clinical care for these patients.
 Video
Video
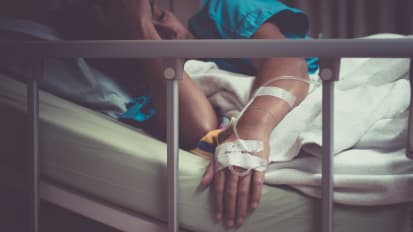
Hospital-Acquired Infections and the OB/GYN Patient
Paul Pottinger, MD, FIDSA, provides an update on the current situation with HAIs, SSI, Influenza, Legionella, MRSA, & C.difficile in cesarean sections and hysterectomy.
 Video
Video
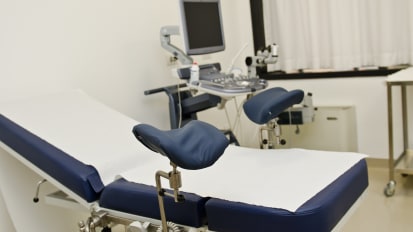
Trauma-Informed Care for the Obstetrician-Gynecologist
Lauren Owens, MD, MPH, defines trauma and trauma-informed care, describes the prevalence of trauma among various populations, describes a trauma-informed approach to the pelvic exam and informs of a trauma-informed approach to labor and delivery.
 Video
Video
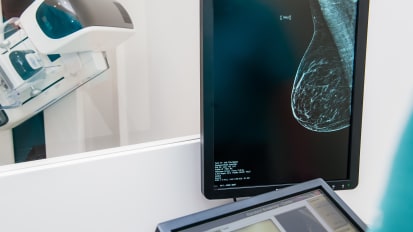
Prostate and Breast Cancer Issues in Screening and Management
Jonathan Wright, MD discusses the similarities between Prostate and Breast Cancer, including screening controversies & USPSTF, treatment paradigms & active surveillance for low risk disease, and BRCA mutations & how they are important for prostate cancer.
 Video
Video
Post-Treatment Gyn Cancer Survivorship Care: Perceptions, Approach, and the Future
Jovana Martin, MD, MPH, reviews trends in increasing prevalence in cancer survivors. She also provides a review of surveillance methods for gynecological cancers and helps to understand the late effects of cancer treatment.
 Video
Video
Delayed Cord Clamping for Preterm & Term Infants
Shani Delaney, MD, discusses delayed cord clamping for preterm and term infants.
 Video
Video
Partnership Access Line (PAL) for Moms
PAL for Moms, formerly the Perinatal Psychiatry Consultation Line, is a free service where any WA state provider caring for a pregnant or new mom with mental illness can receive advice from a UW psychiatrist.
 Video
Video
Microbirth: Vaginal Microbes, Mode of Delivery and Establishing the Infant Gut Microbiota
Caroline Mitchell, MD, MPH, discusses what gut microbes have to do with chronic diseases such as diabetes, IBD, obesity, asthma, etc. Where do our bacteria come from? What is the bacteria we begin life with?
 Video
Video
Rebecca Taub, MD, MPH, provides an update on current governmental initiatives targeting women and reproductive rights. She describes several fast, easy and effective strategies for activism and resistance.
 Video
Video
Adolescent Health: Eating Disorders
Yolanda Evans, MD, MPH, talks about eating disorders, using cases to give examples of how to diagnose, identify signs and symptoms, complications and treatment approaches.
 Video
Video
Implications of Maternal-Fetal Exchange
Hilary Gammill, MD, discusses the implications of maternal transfer to the fetus; implications of feto/placental transfer to the mother; reproductive origins of maternal disease and evolutionary context.
 Video
Video
Unsafe Abortion: Past, Present, and Future
Elizabeth Harrington, MD, describes the epidemiology of unsafe abortion in the global setting and explains how legal restrictions on abortion affect quality of care.
 Video
Video
The Zika Virus Epidemic and Effects on the Fetal Brain
Kristina Adams Waldorf, MD covers many aspects of the significant and enduring public health challenge of the Zika Virus.
 Video
Video
Treating Symptoms of Menopause in Women with Gynecologic Cancer
Tiffany Beck, MD, MPH, gives a review of menopause and health in the well woman and how it overlaps with the cancer survivorship population.
 Video
Video
But It's LEGAL! The Data on Marijuana Use in Pregnancy & How to Counsel Patients Who Use
Timothy Mitchell, MD, talks about the history of marijuana, legalization, its targets and how it is consumed.
 Video
Video
Unraveling the Complexities of "Rh" in Pregnancy
Swati Shree, MD, MHA, discusses the Rhesus system, Pathogenesis, screening, diagnosis and prevention of RhD alloimmunizaton. Dr. Shree also explains anti-D lg, unique scenarios and other national guidelines. She lastly discusses fetal RHD genotyping.
 Video
Video
Pregnancy and the Obese Gravida
Suchi Chandrasekaran, MD, MSCE, reviews the effects of obesity on pregnancy and novel approaches to care. She also discusses the risks, or maybe benefits, of pregnancy on obesity.
 Video
Video
Urgency Urinary Incontinence: Evaluation and Management
Anna Kirby, MD, gives an overview to understand the initial evaluation of urinary incontinence, when to refer and the treatments for urgency urinary incontinence.
 Video
Video
Amies Oelschlager, MD, helps one understand the outcomes of dilation versus surgery, learn to assess for readiness and know how to teach dilation therapy and troubleshooting techniques.
 Video
Video
David Eschenbach, MD, reviews the pathophysiology and treatment of sepsis during pregnancy and discusses different treatment options.
 Video
Video
Is It Prime Time for Primary HPV Screening?
Connie Mao, MD, explains HPV screening and interim guidelines.
 Video
Video
Managing Perinatal Mood Disorders
Deb Cowley, MD, discusses the prevalence and significance of mood disorders during pregnancy and postpartum.
 Video
Video
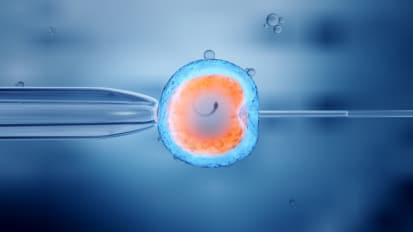
Ethical Issues in Egg Donation
Lorna Marshall, MD, discusses general ethical concepts as they apply to egg donation and some specific issues we now face.
 Video
Video
Identifying Hereditary Ovarian Cancer Risk: An Opportunity to Save Lives
Elizabeth Swisher, MD, Professor, provides an update on identifying the hereditary ovarian cancer risks since this has gone through a major transformation in the recent year.
 Video
Video
Encountering Ovarian Cancer in the Primary Care Setting
Kathryn Pennington, MD, describes the patterns of care in treating ovarian cancer, while identifying women who are at risk.
 Video
Video
Urogynecology For the Primary Care Provider
Cindi Lewis, MD, provides an overview of how to manage patients with urinary incontinence, and learn conservative management of fecal and urinary incontinence.
 Video
Video
Sandura Juul, MD, PhD, presents at the Neurology Grand Rounds on Neonatal Neuroprotection. She reviews the background on Erythropoietin (Epo), neonatal mortality statistics, therapies, treatments, and clinical trials.
 Video
Video
Saving Babies at UW Medical Center: The Pitkin Family's Story
In May 2011, Gretchen Pitkin delivered triplets at UW Medical Center's Neonatal Intensive Care Unit. The three babies were in the NICU for various lengths of time, one for 100 days. They are now 15 months old and are thriving. Watch their amazing story.
 Video
Video
Neonatal Intensive Care at the UW Medical Center Montlake Tower
UW Medical Center's Neonatal Intensive Care Unit is one of our greatest prides.
 Video
Video
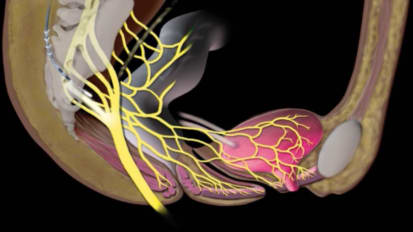
2016 Fertility Evaluation and Management: An Opportunity for Precision Medicine
Genevieve S. Neal-Perry MD, PhD, discusses fertility evaluation and management for couples or individuals looking to start a family.
 Video
Video
New Treatment Options for Accidental Bowel Loss
Michael Fialkow, MD, MPH, gives an overview of the epidemiology and risk factors in fecal incontinence, then discusses management options for this condition.
 Video
Video
Mitochondrial (Genome) Replacement Therapy: The Harbinger of All Things Future
Eli Y. Adashi, MD, focuses on diseases that derive from Mutant Mitochondrial DNA (mtDNA).
 Video
Video
Navigating the Genome: Applications of Genomic Medicine in OB/GYN & Public Health
Jim Evans, MD, discusses application of genomic medicine in the OB/GYN Clinic and in public health.
 Video
Video
Dr. Kristina Adams Waldorf - Preventing Preterm Birth initiative
New innovative research projects aiming to prevent premature birth have been announced by the Global Alliance to Prevent Prematurity and Stillbirth (GAPPS), an initiative of Seattle Children's.
 Video
Video
HPV and Cervical Cancer: 25 Years from Discovery to Vaccine
Denise Galloway, PhD, shares the natural history of genital HPV infection and evidence for their role in cancers, mechanisms by which HPVs contribute to cancer, and the development of vaccine to prevent HPV infection.
Protocols & Guidelines
 Document
Document
Maternal Cardiopulmonary Protocol: Recognition and Initial Evaluation
University of Washington Medical Center Maternal Cardiopulmonary Protocol provides a summary of symptoms and signs, differential diagnosis and initial evaluation steps.
 Document
Document
Inpatient Thromboprophylaxis in Pregnancy and Postpartum
OB Consensus Statement on practice guidelines for hospital antepartum and postpartum services, reviewing indications for inpatient pharmacologic prophylaxis against thromboembolism.
 Document
Document
Gestational Diabetes: Screening Strategies, Glycemic Targets and Pharmacologic Management
Obstetric Consensus Conference, August 2019
 Document
Document
Vaginal Preparation Prior to Cesarean Delivery: Obstetric Consensus Conference
Post-operative infections are the most common cause of postpartum morbidity and significantly affect maternal well-being as well as hospital readmissions.
 Document
Document
Obstetric Consensus Statement, Revised April 2019
 Document
Document
Identification and Management of Sepsis in Pregnancy
Maternal sepsis, especially puerperal sepsis, is a common pregnancy-related condition and in the United States (US) is a leading cause of maternal mortality.
 Document
Document
Anticoagulation Management of Pregnant Women with Mechanical Heart Valves
OB Consensus Statement on Anticoagulation Management of Pregnant Women with Mechanical Heart Valves by maternal fetal medicine and cardiology team at University of Washington Medical Center.
 Document
Document
University of Washington Comment on Arrive Trial Publication - September 2018
University of Washington Comment on ARRIVE Trial Publication, Shani Delaney, M.D. response contact
 Document
Document
Management of Acute Severe Hypertension in Pregnancy
OB Consensus Statement on Management of Acute severe hypertension in pregnancy by maternal fetal medicine team at University of Washington Medical Center
 Document
Document
Tranexamic Acid for Prevention and Treatment of Postpartum Hemorrhage
University of Washington presents the June 2018 Obstetric Consensus Conference. The objective is to evaluate the use of TXA for prevention and treatment of postpartum hemorrhage (PPH) in the obstetric setting.
 Document
Document
Postoperative Obstetric Opioid Prescribing
Recreational use of opioids, the powerful class of analgesic drugs which includes both illicit and prescription medications, has soared over the past two decades.
 Document
Document
Antenatal Steroids For Late Preterm Pregnancies
Antenatal corticosteroids have been widely used in practice for pregnancies at risk for early preterm delivery.
 Document
Document
Management of the Second Stage of Labor
In the United States, cesarean section rates are on the rise. Active management of labor throughout the first and second stage can help early identification of problems to guide practitioners in adjusting modifiable factors.
 Document
Document
Cesarean Delivery Enhanced Recovery CareMap
How to prepare for a Cesarean Delivery and what to expect.
 Document
Document
Perioperative Management of the Obese Parturient - Obstetric Consensus Conference
The purpose of this consensus statement is to provide perioperative guidelines that need to be considered when performing a cesarean section in an obese gravida.
 Document
Document
Manual Vacuum Aspiration for Early Pregnancy Loss: Managing Complications
Training, Education & Advocacy in Miscarriage Management
 Document
Document
OBBE Bleeding Emergency Protocol
Management of OB Hemorrhage and OBBE (OBstetric Bleeding Emergency): 08/06/15
Information & Resources
 Document
Document
Eastern Washington Women's Health Medical Conference
UW Medicine sponsored Conference in Moses Lake, Washington on October 11 & 12, 2019.
 Document
Document
New Opportunities for the Assessment of Preterm Birth
In the present study, we report a community resource that includes "omics" data from approximately 12,000 samples as part of the integrative Human Microbiome Project.
 News
News
Decreasing Hospital Stay and Cost After Cesarean Delivery
Implementation of an ERAS pathway for women having planned or unplanned cesarean delivery was associated with significantly decreased postoperative length of stay and significant direct cost-savings per patient, without an increase in hospital readmissions.
 News
News
The UW Medicine Center for Women & Children: Discover Seattle's Best Kept Secret
UW Medicine has some of the highest success rates in the region for the care of gynecologic cancer, high-risk obstetrics, infertility, family planning and pelvic health issues.
 News
News
Measles Q&A: Pediatrician Fields Common Queries
Responding to the state outbreak, Beth Ebel, MD, discusses the vaccinations, dosages, herd immunity, age requirements, and more.
 Document
Document
Maternal HTN Clinic Referral Protocol
UW Medicine guidelines for making a referral to the Maternal Hypertension Program at the Center for Women & Children.
 News
News
Sex, Drugs & Cranberry Juice: What You Need to Know About UTIs
Ann Stapleton, MD, shares her expertise in chronic UTIs in women in this patient information article.
 Document
Document
Pregnancy & Childbirth Brochure
Choosing a care provider for pregnancy is a personal decision. Many women choose an obstetrician-gynecologist to manage their pregnancy and delivery.
 Document
Document
If You Have a High-Risk Pregnancy: Brochure for Patients
This brochure explains services and providers at 2 UW Medicine clinics: the Maternal and Infant Care Clinic at UW Medical Center (UWMC) and the Maternal Fetal Medicine Clinic at Valley Medical Center.
 Document
Document
For more than 50 years, the skilled and compassionate neonatal professionals at UW Medicine have been dedicated to providing the highest level of care for even the most fragile newborns and their families.
 Document
Document
Neonatology Overview for Families
UW Medicine is proud to offer the two highest levels of care (levels III and IV) in our NICUs.
 Document
Document
Meet UW Medicine's team of Neonatologists who have been delivering the highest level of care to infants born prematurely and/or with physical and genetic anomalies for over 50 years.
 Document
Document
The UW Medicine gynecologic oncology team at University of Washington Medical Center consists of nationally recognized healthcare professionals with extensive clinical knowledge and surgical expertise to prevent and treat cancers.
 Document
Document
Gynecologic Cancer Care: Meet Our Team
UW Medicine gynecologic oncology experts work with patients to prevent and treat complex gynecologic cancers.
 Document
Document
Pelvic Health Center Clinical Overview
The UW Medicine Pelvic Health Center provides comprehensive and compassionate patient-centered care for routine and complex pelvic floor conditions.
 Document
Document
Meet Our Pelvic Health Center Team
The UW Medicine Pelvic Health Center draws on experienced specialists across several medical and surgical domains so that each patient may benefit from multiple knowledgeable perspectives to determine the best course of care.
 Document
Document
UW Medicine’s maternal fetal medicine specialists consult on complex medical conditions of the mothers such as diabetes, hypertension and diseases of the heart, kidneys, lungs and immune system.
 Document
Document
High-Risk Pregnancy Consultation
UW Medicine obstetrics is dedicated to the health and well-being of women and their babies.
Research & Publications